What is Keratosis pilaris?
Keratosis Pilaris (KP): Symptoms, Causes, Treatment & Daily Management for Smoother Skin
If you’ve noticed rough, bumpy “chicken skin” on your upper arms, thighs, or cheeks that feels like sandpaper, you’re likely dealing with keratosis pilaris (KP). This extremely common, harmless skin condition affects up to 80% of children and teens and about 40% of adults. Also called “chicken skin,” KP is not contagious, not dangerous, and often improves significantly by age 30.
This patient-focused guide is optimized for people searching “keratosis pilaris treatment,” “how to get rid of chicken skin,” or “KP on arms and thighs.” It delivers clear, actionable advice to help you manage symptoms and achieve smoother, more confident skin.
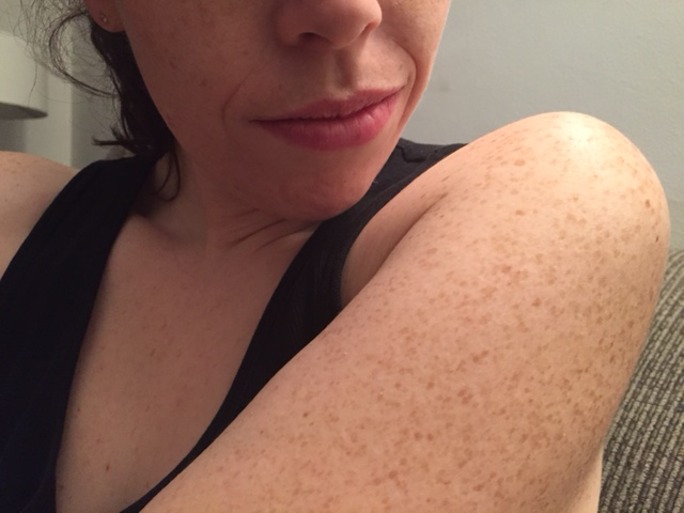
It is most often found on the lateral upper arms and on the front of the thighs. The buttocks and face are occasionally involved. Keratosis pilaris causes the skin to have a sand paper-like feeling. Occasionally, red halo surrounds the white “spike”.
The lesions are located at the openings of the hair follicles and often can be scooped out with a fingernail or an instrument called a dermal curette. When this is done, a coiled hair is sometimes found within the white semi-solid material. These spots usually return. The individual spots come and go over a matter of weeks, but the overall course of this condition is chronic. The good news is that this condition gradually disappears, usually after age twenty.
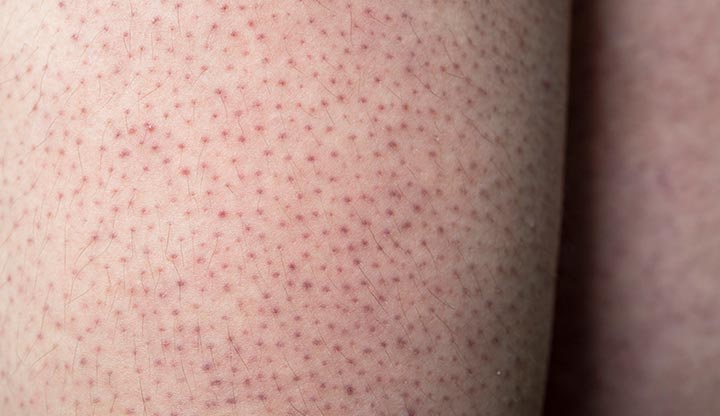
What Are the Symptoms of Keratosis Pilaris?
Keratosis pilaris appears as clusters of tiny, firm, rough bumps (1mm or smaller) around hair follicles. These bumps are usually:
- Skin-colored, white, red, pink, or brownish (depending on skin tone)
- Located on the upper outer arms, front of thighs, buttocks, or cheeks (in children)
- Accompanied by dry, sandpaper-like texture
- Sometimes surrounded by a faint red halo or mild itching, especially in dry weather
Symptoms often worsen in winter due to low humidity and improve in summer. The bumps are painless for most people but can affect self-esteem due to their appearance.
Causes and Who Gets Keratosis Pilaris
KP occurs when keratin (a natural skin protein) builds up and plugs hair follicles instead of shedding normally. It’s strongly genetic—often runs in families—and commonly linked to dry skin or conditions like eczema (atopic dermatitis).
Risk factors include:
- Childhood and teenage years
- Fair skin or atopic background
- Dry climates or winter months
- Family history
It’s not caused by poor hygiene or diet and cannot be “cured,” but symptoms are highly manageable.
How Is Keratosis Pilaris Diagnosed?
A board-certified dermatologist can usually diagnose KP with a simple visual exam—no biopsy is typically needed. They’ll rule out similar conditions like acne, eczema, or folliculitis. Early evaluation helps create an effective personalized plan, especially if redness or itching is prominent.
Living with Keratosis Pilaris: Proven Daily Management Tips
Take control with these practical habits that many patients swear by:
- Apply moisturizer immediately after bathing while skin is damp
- Use gentle, soap-free cleansers (Cetaphil, Dove Sensitive)
- Wear loose, breathable clothing to reduce friction
- Use a humidifier in dry indoor environments
- Avoid harsh scrubbing or picking at bumps (this worsens irritation)
- Protect skin with sunscreen daily—sun exposure can sometimes highlight redness
- Track flares in a journal to identify seasonal or environmental triggers
For children with facial KP, gentle care prevents self-consciousness as they grow. Most see major improvement with age plus consistent skincare.
When to See a Dermatologist for Keratosis Pilaris
Schedule an appointment if:
- Bumps become itchy, red, or inflamed
- Home care isn’t helping after 6–8 weeks
- You want faster cosmetic improvement
- KP affects your confidence or quality of life
Dermatologists can tailor advanced treatments for stubborn cases.
Frequently Asked Questions About Keratosis Pilaris
Does keratosis pilaris go away? Often improves or resolves by adulthood, especially after age 30, but can persist mildly.
Best cream for KP? Look for urea, lactic acid, or salicylic acid formulas applied consistently.
Is KP the same as acne? No—KP is keratin plugs, not oil or bacteria-related like acne.
Can diet help keratosis pilaris? No direct link, but staying hydrated and eating omega-rich foods supports overall skin health.
Is keratosis pilaris contagious? Absolutely not—it’s a genetic skin variation.